100000 IU vitamin D monthly helps COPD patients – 3 RCT
Vitamin D Improves Exercise Outcomes In Patients With COPD
Medical News Today, 16 May 2011
Vitamin D supplements may help patients with chronic obstructive pulmonary disease (COPD) get more from their pulmonary rehabilitation programs, according to a study conducted by researchers from Belgium.
The study results will be presented at the ATS 2011 International Conference in Denver.
"Our study shows that high doses of vitamin D supplementation on top of a standard rehabilitation program improve the outcome in terms of exercise capacity and respiratory muscle strength," said Miek Hornikx, physiotherapist and doctoral student in the department of pneumology at the Katholieke Universiteit Leuven in Leuven, Belgium.
Vitamin D deficiency is common among patients with COPD, and is often associated with lack of exposure to sunlight and diet. COPD patients also often have limited physical activity as a result of breathing difficulties associated with the disease, which also may result in less exposure to sunlight, Ms. Hornikx explained.
"COPD can be considered as a respiratory disease with important non-respiratory consequences, such as osteoporosis, cardiovascular disease and muscle weakness," she said. "These consequences eventually will be negatively influenced by physical inactivity which, along with exercise intolerance, is a common feature among patients with COPD and is proven to be related to mortality.
"Low levels of vitamin D in the blood have been related with muscle weakness, a major target for respiratory rehabilitation and increased risk of falls," she added "Since vitamin D is often depleted in patients with COPD, we wanted to see if vitamin D supplementation would have a beneficial effect on rehabilitation among these patients, perhaps by increasing muscle strength."
The researchers enrolled 50 COPD patients with a history of exacerbations who had been referred for rehabilitation and randomly assigned them to receive either a monthly dose of vitamin D or placebo. Patients in the vitamin D group were given 100,000 IUs (international units) of vitamin D in their monthly dose ; the U.S. recommended daily allowance of vitamin D is 600 IUs daily for adults up to age 70 and 800 IUs daily for adults over age 70.
All patients participated in a pulmonary rehabilitation program for three months. At the beginning of the study and again at the completion of the rehabilitation program, peripheral and respiratory muscle strength, exercise capacity and vitamin D levels were measured. Patients were also asked to complete a quality of life survey both before and after rehabilitation.
At the end of the study, researchers found that patients treated with vitamin D had a significant improvement in exercise capacity and respiratory muscle strength compared to those in the placebo group.
"These results support the idea that correcting vitamin D deficiency by adding vitamin D supplements to training programs allows COPD patients to achieve better results from rehabilitation, including improvements in muscle strength and exercise capacity," Ms. Hornikx said.
Interestingly, despite significant improvements in exercise capacity in patients treated with vitamin D, those patients did not report a significant increase in health-related quality of life.
"This could be due to the fact that we had a relatively small number of patients included in this study, as well as to the relatively brief duration of the study," Ms. Hornikx said. Future studies should focus on the specific mechanisms by which vitamin D affects patients with COPD, she added.
"Vitamin D Supplementation During Rehabilitation In Patients With Chronic Obstructive Pulmonary Disease: An Intervention Study" (Session B17, Monday, May 16, 8:15-10:45 a.m., Room 201-203 (Street Level), Colorado Convention Center; Abstract 17477)
COPD helped by 100,000 IU vitamin D monthly - RCT
High Doses of Vitamin D to Reduce Exacerbations in Chronic Obstructive Pulmonary Disease: A Randomized Trial
An Lehouck, PhD; Chantal Mathieu, MD, PhD; Claudia Carremans, MS; Femke Baeke, PhD; Jan Verhaegen, MD, PhD; Johan Van Eldere, MD, PhD;
Brigitte Decallonne, MD, PhD; Roger Bouillon, MD, PhD; Marc Decramer, MD, PhD; and Wim Janssens, MD, PhD
From University Hospitals Leuven, Leuven, Belgium.
PDF is attached at the bottom of this page
Background: Low serum 25-hydroxyvitamin D (25-[OH]D) levels have been associated with lower FEV1, impaired immunologic control, and increased airway inflammation. Because many patients with chronic obstructive pulmonary disease (COPD) have vitamin D deficiency, effects of vitamin D supplementation may extend beyond preventing osteoporosis.
Objective: To explore whether supplementation with high doses of vitamin D could reduce the incidence of COPD exacerbations.
Design: Randomized, single-center, double-blind, placebo-controlled trial. (ClinicalTrials.gov registration number: NCT00666367)
Setting: University Hospitals Leuven, Leuven, Belgium.
Patients: 182 patients with moderate to very severe COPD and a history of recent exacerbations.
Intervention: 100 000 IU of vitamin D supplementation or placebo every 4 weeks for 1 year.
Measurements: The primary outcome was time to first exacerbation.
Secondary outcomes were exacerbation rate, time to first hospitalization, time to second exacerbation, FEV1, quality of life, and death.
Results: Mean serum 25-(OH)D levels increased significantly in the vitamin D group compared with the placebo group (mean between-group difference, 30 ng/mL [95% CI, 27 to 33 ng/mL]; P < 0.001). The median time to first exacerbation did not significantly differ between the groups (hazard ratio, 1.1 [CI, 0.82 to 1.56]; P = 0.41), nor did exacerbation rates, FEV1, hospitalization, quality of life, and death. However, a post hoc analysis in 30 participants with severe vitamin D deficiency (serum 25-[OH]D levels <10 ng/mL) at baseline showed a significant reduction in exacerbations in the vitamin D group (rate ratio, 0.57 [CI, 0.33 to 0.98]; P = 0.042).
Limitation: This was a single-center study with a small sample size.
Conclusion: High-dose vitamin D supplementation in a sample of patients with COPD did not reduce the incidence of exacerbations.
In participants with severe vitamin D deficiency at baseline, supplementation may reduce exacerbations.
Primary Funding Source: Applied Biomedical Research Program, Agency for Innovation by Science and Technology (IWT-TBM).
100,000 IU monthly helped COPD - RCT Jan 2015
📄 Download the PDF from Vitamin D Life.
100,000 IU monthly works out to an average of just 3,300 IU daily
Paper shows that the people getting vitamin D got to a blood level of 50 ng - seems amazing that the response was so high
100,000 IU monthly helped COPD RCT 2012
Vitamin D supplementation during rehabilitation in COPD: a secondary analysis of a randomized trial.
Respir Res. 2012 Sep 25;13(1):84.
Hornikx M, Van Remoortel H, Lehouck A, Mathieu C, Maes K, Gayan-Ramirez G, Decramer M, Troosters T, Janssens W.
ABSTRACT: RationalePulmonary rehabilitation is an important treatment for patients with Chronic Obstructive Pulmonary Disease, who are often vitamin D deficient.
As vitamin D status is linked to skeletal muscle function, we aimed to explore if high dose vitamin D supplementation can improve the outcomes of rehabilitation in Chronic Obstructive Pulmonary Disease.
MATERIAL AND METHODS: This study is a post-hoc subgroup analysis of a larger randomized trial comparing a monthly dose of 100.000 IU of vitamin D with placebo to reduce exacerbations. 50 Subjects who followed a rehabilitation program during the trial are included in this analysis. We report changes from baseline in muscle strength and exercise performance between both study arms after 3 months of rehabilitation.
RESULTS: Vitamin D intervention resulted in significantly higher median vitamin D levels compared to placebo (51 [44-62] ng/ml vs 15 [13-30] ng/ml; p < 0.001).
Patients receiving vitamin D had significantly larger improvements in
inspiratory muscle strength (-11 +/- 12 cmH2O vs 0 +/- 14 cmH2O; p = 0.004) and
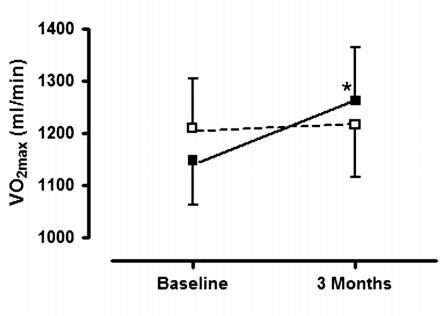
maximal oxygen uptake (110 +/- 211 ml/min vs -20 +/- 187 ml/min; p = 0.029).
Improvements in quadriceps strength (15 +/- 16 Nm) or six minutes walking distance (40 +/- 55 meter) were not significantly different from the effects in the placebo group (7 +/- 19 Nm and 11 +/- 74 meter; p > 0.050).
CONCLUSION: High dose vitamin D supplementation during rehabilitation may have mild additional benefits to training.
PMID: 23006613
Discussion which was extracted from PDF attached to the bottom of this page
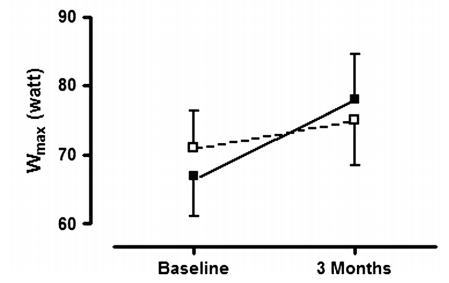
The present study is the first placebo controlled intervention study exploring the effect of supplementation with high doses of vitamin D in a 3 month rehabilitation program in patients with COPD. We found that, compared to training alone, patients receiving a monthly dose of 100.000 IU of vitamin D had a larger improvement on inspiratory muscle strength and peak exercise tolerance. There was a similar trend towards higher quadriceps strength, six minutes walking distance and dyspnea scores, but these effects did not reach statistical significance.
Although the reported effects are rather limited, the current data support the hypothesis that vitamin D supplementation may enhance training effects in disabled patients with muscle weakness and reduced exercise capacity. There are two reasons which may explain why a larger and general benefit could not be found. Most importantly, our data are post-hoc subgroup analyses of a larger randomized controlled trial and therefore not designed nor sufficiently powered to demonstrate clinically significant benefits. Secondly, our training program in the total study group yielded important effects on quality of life and symptoms,
but resulted in somewhat smaller effects than expected on physiological outcomes. As the latter outcomes would be preferentially affected by vitamin D because of common pathways in the muscle [8], the window for improvement under vitamin D was a priori small. The absence of clinically relevant training benefits in quadriceps strength and functional exercise capacity in the total subgroup may reflect the individual variability in training response, especially observed in very disabled COPD. Nevertheless, largest effects were preferentially obtained in the vitamin D supplemented group, whereas the placebo group seemed more resistant to physiological improvements.
Currently, it is still unclear which serum vitamin D levels are needed for an optimal muscle function [7,14,32]. Different intervention studies indicate that vitamin D supplementation may only improve muscle strength when baseline levels are deficient but surprisingly, few studies have explored this question in a context of training [33]. Bunout et al. reported that a daily intake of 400 IU of vitamin D with 800 mg of calcium plus biweekly strength, balance and aerobic exercises in an elderly population did not enhance muscle mass or function compared to either exercise or vitamin D alone [34]. A more recent randomized trial evaluated whether a daily consumption of fortified milk (800 IU of vitamin D and 1000 mg of calcium) enhanced the effects of resistance training in a community dwelling elderly population, but again no significant effect could be found [35]. Different authors therefore suggested that the supplementation dosage of vitamin D in these trials was probably insufficient to obtain potential benefits [14,33]. Our data support this idea as the high dose of vitamin D (corresponding to a daily intake of 3300 IU) increased median 25-OHD levels up-to 51 [44-62] ng/ml in the intervention arm with superior clinical effects compared to placebo. We also evaluated whether larger benefits were present in the subgroup of patients being vitamin D deficient at baseline. No significant relationship could be found but we should acknowledge that these subgroups were probably too small to appreciate any difference.
The effects of vitamin D on the skeletal muscle are either direct on contractility via blood calcium levels, but most are indirectly mediated through the vitamin D receptor (VDR) which is abundantly expressed in the skeletal muscle [36]. Vitamin D deficiency is shown to reduce actin and troponin content, to impair calcium uptake in the sarcoplasmatic reticulum, to down-regulate protein synthesis and to increase apoptosis [8,37], processes which are all described in skeletal muscles of patients with COPD [38-40]. Typically, severe vitamin D deficiency results in a type II fiber atrophy with interfibrillar spaces infiltrated with fat, fibrocytes and glycogen [35]. As skeletal muscles of patients with COPD are characterized by fiber type shifts towards a type II profile, vitamin D deficiency may have a superimposed deleterious effect [37,41]. Since patients with COPD are often vitamin D deficient and frequently suffer from skeletal muscle weakness, they compose an interesting target population for combined intervention studies with vitamin D supplements and training [42]. Currently, a randomized trial specifically designed to study these questions in COPD is ongoing (clinicaltrials.gov. NCT01416701). Our data generate aspiration that a significant and clinical benefit may be revealed.
Overall, the present post-hoc analysis supports the idea that in patients with COPD high dose supplementation with vitamin D can be beneficial when combined with exercise training. Our data should be confirmed by other studies sufficiently powered to evaluate clinical and sustained benefits in patients with COPD or specific subgroups. Only then recommendations on the appropriate use and dosage of vitamin D supplements in a clinical context of training can be made.
Based on published research listed on this page and elsewhere on Vitamin D Life
Start with just 1,000 IU the check for a rare allergic reaction reaction to vitamin D
If no allergic reaction, and there is a chance that you have low vitamin D levels,
- take a loading dose of about 300,000 IU of vitamin D spread out over a month (say 50,000 IU every 5 days)
- A loading dose will ''fill up" the vitamin D levels in the blood
- And probably provide some great positive benefits which will encourage continued supplementation
Maintenance dose of at least 3300 IU daily ( or 50,000 IU every 2 weeks)
After 2-4 months on the maintenance dose, have your Vitamin D blood level tested (approx $40)
- The current research shows that a vitamin D level of at least 50 nanograms/ml is needed to treat COPD
- If your blood level is, say, at only 40 ng, increase your dose by at least 1,000 IU daily, and test again in 3-4 months
- By the way, you might consider another path - taking more vitamin D than necessary (say 10,000 IU daily) then reducing if needed
Note: You should not have large mono-therapies of anything, even vitamin D.
When taking more than about 3,000 IU of vitamin D you should balance your cofactors
Briefly this means:
Reduce total Calcium to 500 mg,
Increase your total Magnesium to 500 mg
Take Vitamin K2 - about 100 mcg
There are many suppliers which have all of the cofactors in a single product - capsule, liquid, and fizzy
Total cost for the vitamin D and cofactors is usually less than 20 cents per day.
See also Vitamin D Life
Search Vitamin D Life for COPD 234 items as of Nov 2013
Lung and Vitamin D – Special Issue Dec 2011 many articles on COPD and Vitamin D
COPD patients 4X more likely to have low Vitamin D – 2 articles in 2012
Breathing and vitamin D items
Severe asthma children 31X more likely to develop chronic obstructive lung disease -May 2010
COPD not treated with 3,300 IU daily average of vitamin D unless very deficient – Jan 2012
- Differs from the conclusion of the abstracts on this page
- COPD 2X as likely if low vitamin D – review of 3 studies – March 2014
See also web
Clinical Trials for COPD and Vitamin D INTERVENTION 20 listed as of Oct 2018
COPD and 5800 IU daily for first 5 weeks, then 3,000 IU daily
COPD at Vitamin D Council which has 49 references
