Brain and Vitamin D - Massive Review - 2026
Vitamin D and Brain Health: A Systematic Review
Clinical Nutrition Open Science https://doi.org/10.1016/j.nutos.2026.100646
Lebanon
Vitamin D, once considered solely important for bone health, is increasingly considered a key neuro-steroid involved in brain development and function. This PRISMA-registered systematic review synthesizes evidence on the association between vitamin D status and neuropsychiatric and neurological disorders and evaluates the effects of vitamin D supplementation on brain-related outcomes. It integrates findings from 90 studies including meta-analyses, clinical trials, and observational studies, about the associations between vitamin D status and the range of neuropsychiatric and neurological disorders. From depression, schizophrenia, and autism spectrum disorders to neurodegenerative disorders such as Alzheimer’s and Parkinson’s, most studies show that low vitamin D is associated with increased risk, increased severity of symptoms, or worse outcomes. Supplementation, particularly for those who are deficient, usually provides improvements resulting in moderate but meaningful improvement in mental health symptoms, neurodevelopmental outcomes, and cognitive function. It is notable and probably most beneficial in individuals with baseline deficiency, and emerging evidence suggests genetic and microbiome factors may impact its benefits. This review emphasizes that vitamin D is a modifiable, low-cost, risk factor for mental and neurological health. This is especially pertinent in vulnerable populations (pregnant individuals; children; aging; psychiatric diagnoses). Vitamin D supplementation cannot be recommended as a primary treatment for neuropsychiatric or neurological disorders, but assessment and correction of deficiency may be considered as part of comprehensive care in selected high-risk populations. The review protocol was registered in PROSPERO (CRD420261282220).
Conclusion - from PDF
Overall, the current systematic review illustrates that vitamin D is a critical modulator in mental and neurological health throughout the lifespan. Low vitamin D levels have been consistently linked with higher risk and severity of mental and neurological disorders, including depression, anxiety, schizophrenia, autism, ADHD, neurodegenerative diseases, and sleep disorders. In many instances, vitamin D deficiencies emerge, not solely in the context of illness, but as a contributing factor to the illness process or outcome. Vitamin D supplementation restores vit D levels with a myriad of favorable clinical outcomes, including improvement of depressive symptoms and antidepressant response, and improvement in socialization in autism, as well as possibly, inhibiting cognitive decline in dementia. Vitamin D's wide-ranging neuro-modulatory mechanisms; downregulating inflammation, neuroprotection, and neurotransmitter production - represents a biological basis for the clinical benefits seen. Table 3 shows the vitamin-D-regulated targets by brain region, and Figure 6 qualitatively synthesizes the genomic and non-genomic pathway connections from cutaneous synthesis to region-specific clinical correlations.The study findings further support several practical suggestions (1) to avoid vitamin D deficiency by obtaining adequate dietary intake and/or supplementation in general and in particular in pregnant women, children and older adults as a worthwhile and low-cost public health approach that may yield neurodevelopmental and neuroprotective benefits; (2) to monitor and treat hypovitaminosis D status in patients with psychiatric or neurological disorders as part of coordinated care. In selected patient populations, particularly those with documented deficiency, vitamin D repletion may improve selected clinical outcomes, vitamin D supplementation will lead to better treatment outcomes and improved physical health, and in some cases, it may diminish disease symptoms; (3) to integrate a vitamin D status assessment into future clinical trials testing mental health intervention, to analyze implications of vitamin D status, and clarify confounding influences of vitamin D deficiency on treatment resistance/response (e.g. ensuring depressed patients are not severely Vitamin D deficient or investigating if patients with Vitamin D deficiency can achieve greater benefits from certain interventions).
In conclusion, Vitamin D is a modifiable filter through which we navigate the complex matrix of brain health. No single item or factor will remediate imbalanced factors related to mental and neurological disorders, as these conditions arise from a variety of complex origins, which is precisely why all of the unique sensors and manipulations are necessary to drive improvements over the whole lifespan of the person. That said, by improving Vitamin D status at the population and clinical levels, we may attain a modest but meaningful improvement in mental well-being and neurological function. The evidence collected in this review clearly suggests that quality attention to the “sunshine vitamin” is part of achieving optimal mental health outcomes and providing support in both preventive and therapeutic capacities. Research will in time be pruned more exquisitely, but in terms of the knowledge base, there is enough evidence to warrant a proactive strategy for maintenance of vitamin D for brain health.
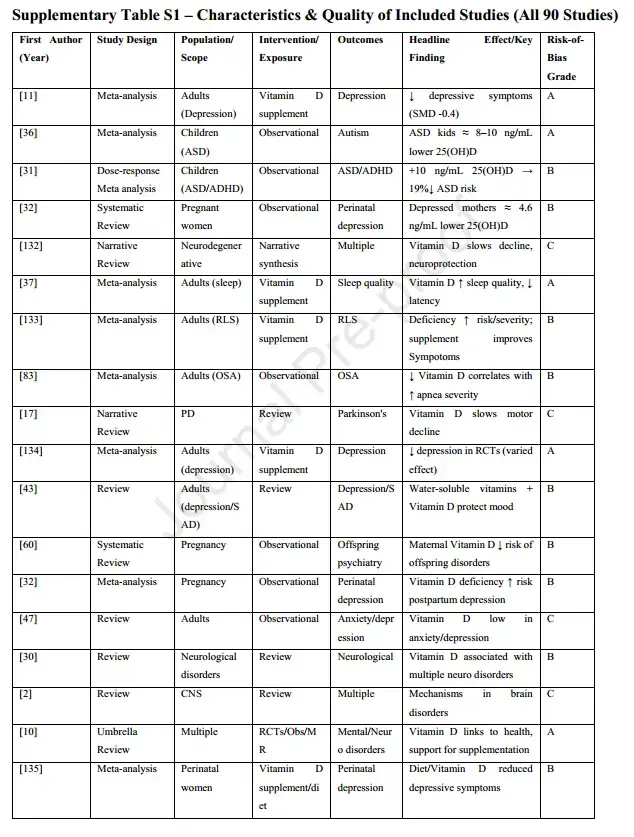
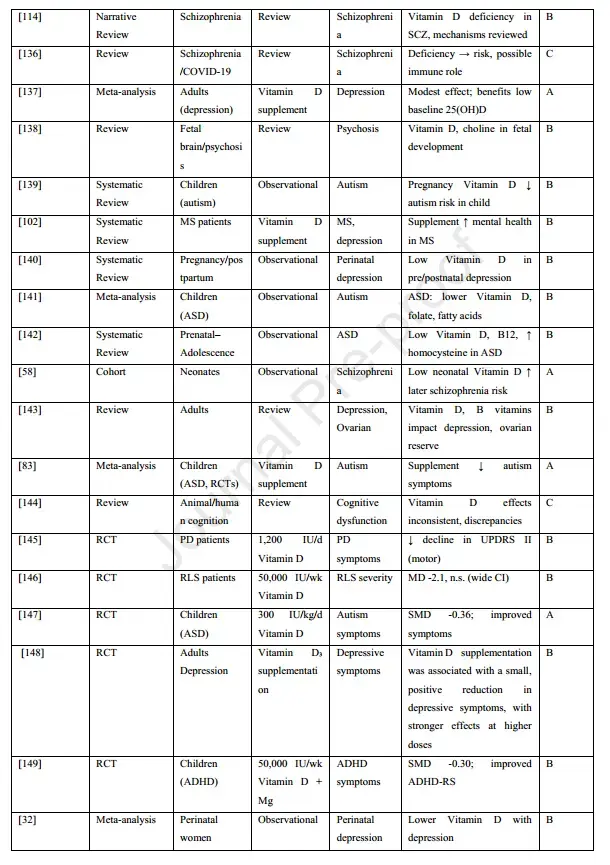
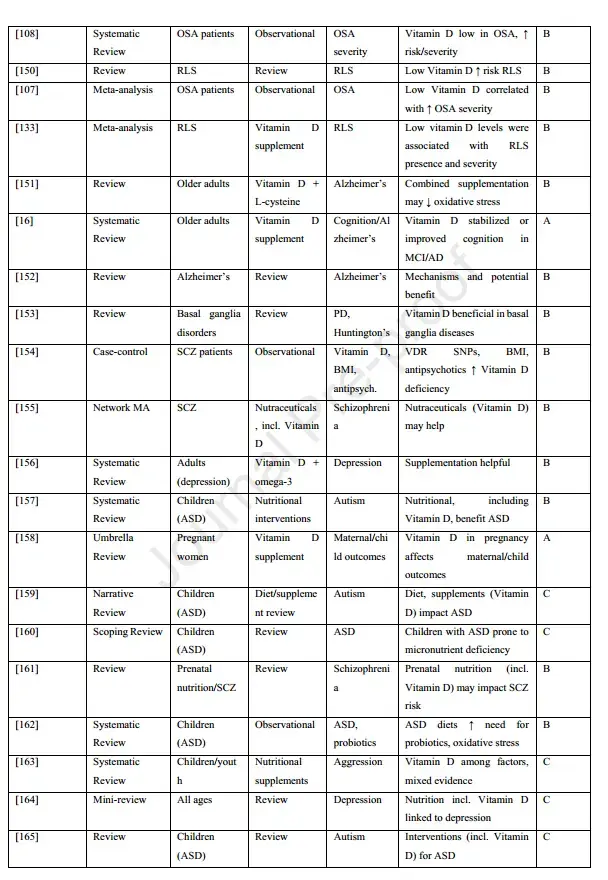
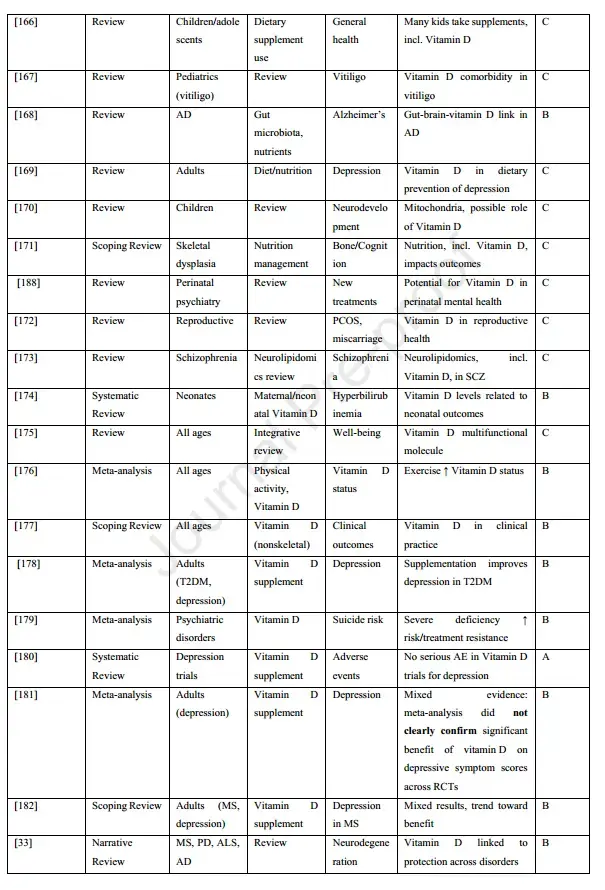
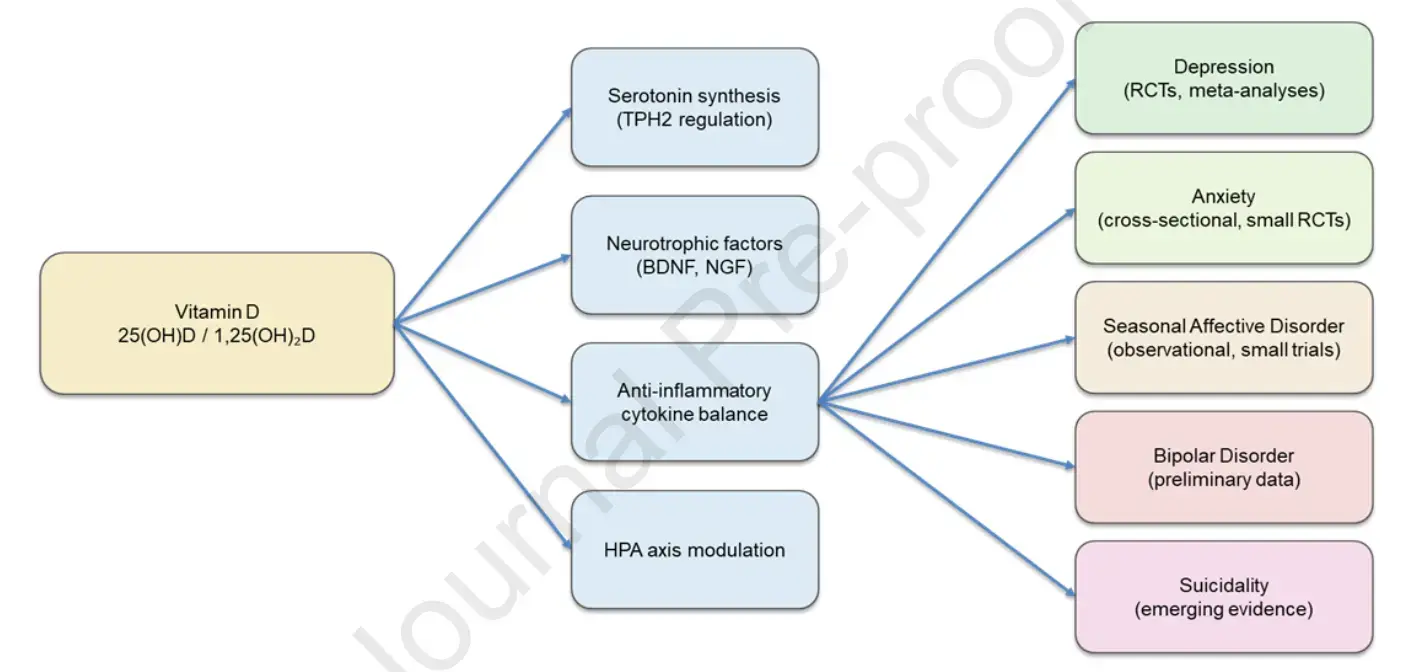
Overview of 90 studies