Depression fought by Vitamin D - yet another meta-analysis
Efficacy of vitamin D supplementation in patients diagnosed with depression: a dose-response meta-analysis of randomized controlled trials
Front Nutr. 2026 Mar 17:13:1772451. doi: 10.3389/fnut.2026.1772451
Background: Depression affects 5% of the global population, posing significant health and economic challenges.
Objectives: This study evaluates the efficacy of vitamin D supplementation in reducing depressive symptoms and explores its dose-response relationship.
Methods: We used PubMed, EMBASE, and Cochrane Library to identify randomized controlled trials using the keyword combination of vitamin D and depression from inception to June 2024. The primary outcome was the change in depressive symptoms. A dose-response meta-analysis using restricted cubic splines was conducted to explore potential sources of heterogeneity and examine the dose-response relationship.
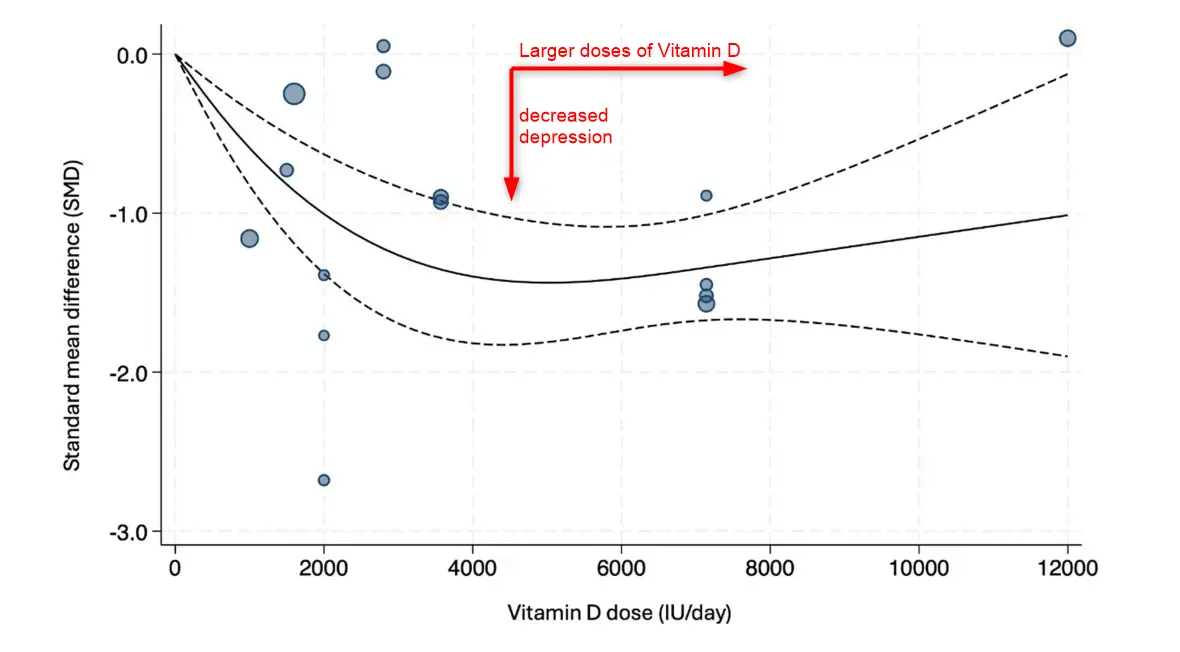
Results: The outcomes were reported in 15 studies encompassing data from 962 participants. Vitamin D supplementation demonstrated a significant improvement in depressive symptoms compared to the placebo group (SMD: -0.98; 95% CI - 1.28 to -0.68; p < 0.001). Statistical heterogeneity was high (I2 = 79%; p < 0.001). Secondary outcomes revealed significant reductions in serum PTH (MD: -4.19; 95% CI - 8.18 to -0.2 pg./mL) and TNFα levels (MD: -0.3; 95% CI - 0.44 to -0.16 pg./mL) in the intervention groups, while other outcomes, such as BMI, weight, and IL-6, showed no significant changes. Dose-response analysis further highlighted that higher daily doses of vitamin D, particularly up to 5,000 IU/day, were associated with the greatest reduction in depressive symptoms.
Conclusion: Our findings from this systematic review and meta-analysis indicated that vitamin D supplementation may be an effective adjunctive therapy for improving depressive symptoms. The observed reductions in serum PTH and TNFα levels suggest anti-inflammatory mechanisms underlying its antidepressant effects. Higher daily doses, particularly around 5,000 IU, were associated with greater symptom improvement within the studied populations.
