Pancreatic Cancer needs more than Vitamin D monotherapy - March 2026
Impact of Vitamin D Status on Pancreatic Cancer Risk and Outcomes
Nutrients 2026, 18, 837 https://doi.org/10.3390/nu18050837
Beata Jablonska * and Slawomir Mrowiec – Poland
Vitamin D (VD), a fat-soluble prohormone, exerts diverse effects on cellular proliferation, differentiation, and immune modulation, with accumulating evidence supporting its role in pancreatic ductal adenocarcinoma (PDAC) biology. Experimental studies demonstrate that VD and its analogs can inhibit PDAC cell growth and remodel the tumor microenvironment, potentially contributing to tumor suppression. Epidemiological data indicate that VD deficiency is prevalent among PDAC patients and is associated with increased inflammatory biomarkers and reduced overall survival, particularly in early-stage disease. However, meta-analyses reveal inconsistent associations between circulating 25-hydroxyvitamin D levels and PDAC incidence, while higher levels may be linked to improved survival but not reduced risk of disease onset. The clinical utility of VD supplementation for PDAC prevention or treatment remains uncertain, with ongoing debate regarding optimal dosing, timing, and patient selection. This narrative review synthesizes current evidence on the mechanistic, epidemiological, and clinical relevance of VD in PDAC. Particular emphasis is placed on existing knowledge gaps and the need for well-designed clinical trials to clarify the potential therapeutic and prognostic role of VD in pancreatic cancer.
Summary and Conclusions
Despite compelling pre-clinical evidence supporting anti-tumorigenic effects of VD in PDAC, its clinical relevance remains uncertain.
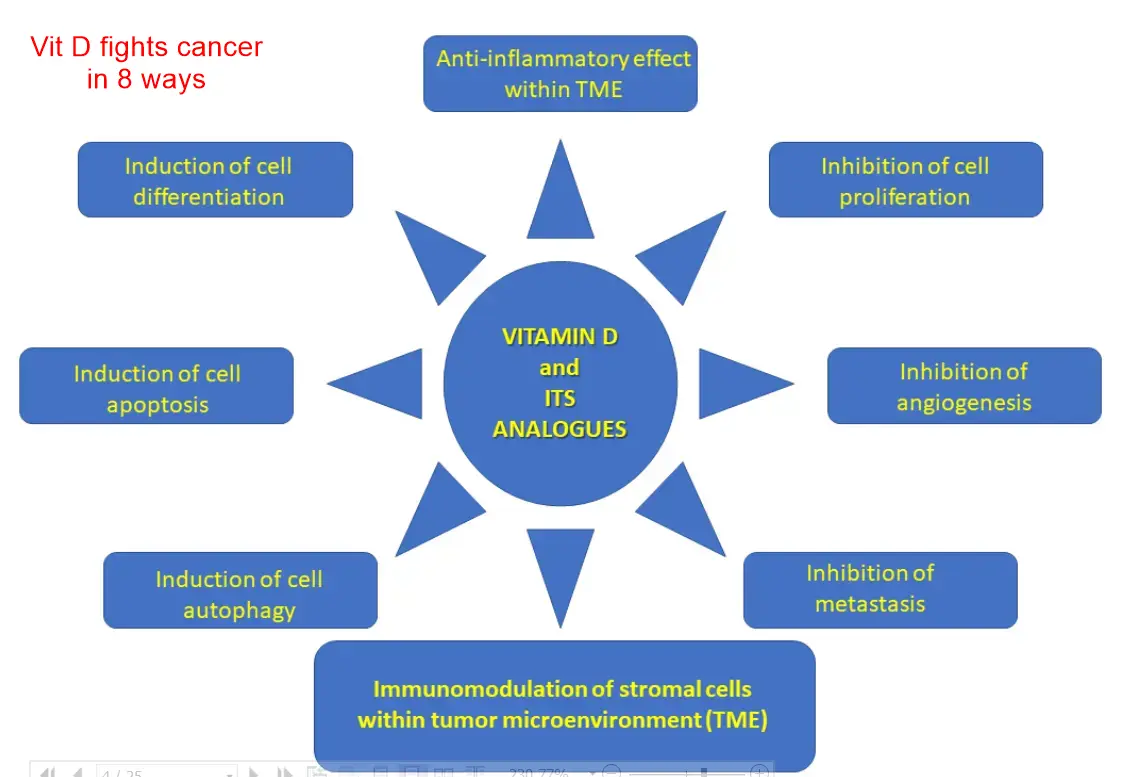
Experimental studies consistently demonstrate inhibitory effects of
- VD on PDAC cell proliferation,
- induction of differentiation,
- modulation of the tumor microenvironment, and
- immune regulation.
However, translation of these findings into clinical benefit has proven challenging.Epidemiological and clinical studies evaluating the association between VD status and PDAC risk or outcomes yield inconsistent results. Observational studies report heterogeneous associations between circulating 25-hydroxyvitamin D [25(OH)D] concentrations and PDAC incidence or survival, while evidence derived from dietary intake and supplementation studies is similarly inconclusive. Some pooled analyses suggest improved survival at moderate VD levels, whereas others report null associations or increased risk at higher concentrations. Large randomized controlled trials have not demonstrated a clear preventive or therapeutic benefit of VD supplementation, likely reflecting methodological heterogeneity, inclusion of VD-replete populations, variability in dosing regimens, and substantial interindividual differences in VD metabolism.
Importantly, emerging evidence suggests that both low and high circulating 25(OH)D concentrations may be unfavorable, supporting a non-linear relationship between VD status and cancer risk.
Population-specific differences in VD metabolism, genetic background, baseline exposure, obesity, smoking status, and comorbidities further complicate interpretation and may partly explain discrepant findings across studies.
Overall, the current evidence is insufficient to support VD supplementation beyond standard recommendations for PDAC prevention or treatment. The available data should be regarded as hypothesis-generating rather than practice-changing, and routine use of high-dose VD supplementation for PDAC cannot be recommended at present. Future research should prioritize well-designed, adequately powered randomized trials with careful stratification by baseline VD status, standardized assessment of 25(OH)D concentrations, and consideration of genetic and metabolic variability. Exploration of VD analogs with improved safety profiles and evaluation of VD as an adjunct to established systemic therapies may further clarify its potential role in PDAC
Related in Vitamin D Life
need to also change gene activation and perhaps add Mg, Vit K, and/or Omega-3
- People consuming more Vitamin K1 were 40 percent less likely to get Pancreatic Cancer
- Pancreatic Cancer risk increased 24 percent for every 100 mg less of Magnesium intake
- Omega-3 should help Pancreatic Cancer in 5 ways
- Vitamin D intake and mortality of 5 cancers: breast, colorectal, lung, pancreatic, and prostate - umbrella
Genes
- Pancreatic Cancer massively deregulates the local Vitamin D receptors and CPY24A1
- Pancreatic Cancer protects itself deactivating HNF4A (which can be reactivated by the Vitamin D Receptor)
- Pancreatic Cancer association with PRKCA gene and the active form of vitamin D
- 8 Vitamin D Receptor activators can fight Pancreatic Cancer
