Vitamin D and exercise after hip fracture surgery – far fewer deaths
Impact of 3-monthly vitamin D supplementation plus exercise on survival after surgery for osteoporotic hip fracture in adult patients over 50 years: A pragmatic randomized, partially blinded, controlled trial
Journal of nutrition, health & aging, pp 1-8, July 2016 https://doi.org/10.1007/s12603-016-0773-3
88 osteoporotic hip fracture patients
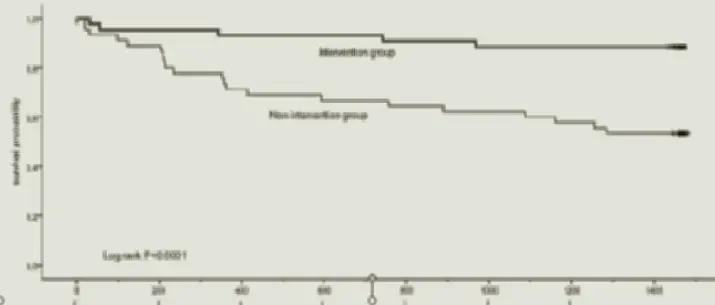
Analysis of Deaths
| 3-monthly oral doses of 3 mg calcifediol + exercise | Placebo | |
| 1 year | 1% | 10% |
| 4 year | 3.4% | 19.3% |
Note: Calcifediol = calcidiol = 25-hydroxycholecalciferol = 25-hydroxyvitamin D = 25(OH)D)
Wonder why they used Calcifediol. Vitamin D works as well if liver is OK and is far less expensive
Wonder why they used 3 monthly dosing. every 20 days is far better
Objective: To determine whether 3-monthly supplementation of an oral vitamin D widely used in Spain (calcifediol) plus daily exercise could influence survival at one and four years after surgery for osteoporotic hip fracture.
Design: A pragmatic, randomized, partially single-blind placebo-controlled study.
Setting: Patients admitted to a tertiary university hospital for acute hip fracture.
Participants: 675 healthy adult patients undergoing surgery for osteoporotic hip fracture were recruited from January 2004 to December 2007.
Intervention: Patients were randomized to receive either 3-monthly oral doses of 3 mg calcifediol (Hidroferol Choque®) or placebo in the 12 months postsurgery. Patients who received calcifediol were also given an exercise programme. The placebo group received standard health recommendations only. Measurements: The primary endpoint was survival at 1 year and at 4 year follow-up. We also recorded new fractures, medical complications and anti-osteoporotic treatment compliance.
Results: We included a total of 88 patients, aged 62 to 99 years. Mean age was 82 years and 88.6% were women. At 12 months, 10 (11.3%) patients had died, 9 of them, from the non-intervention group. At 4 years after surgery, 20 (22.7%) had died, 3 (3.4%) from the intervention group and 17 (19.3%) from the non-intervention group. At this time, survival curve analysis showed 93% survival in the intervention group and 62% in the non-intervention group (p=0.001). At 12-month follow up, there were 18 new fractures, 9 in each group. The non-intervention group had more medical complications, with significant differences at visit 2 (p = 0.04) and 3 (p = 0.02) but not at visit 4 (p = 0.18). No significant differences between groups were found regarding treatment compliance.
Conclusion: 3-monthly, oral supplements of 3 mg calcifediol plus daily exercise improved survival at one-year and four-year follow-up after surgery for an osteoporotic hip fracture.
Secondary hip fractures probably prevented by Vitamin D - meta-analysis March 2026
Secondary fracture risk after hip fracture in older patients: an updated sex-specific systematic review and meta analysis with GRADE and PAF assessment
Osteoporos Int. 2026 Mar 12. doi: 10.1007/s00198-026-07949-z PDF behind paywall
Jiachen Ren # 1 2 3, Mengyuan Liu # 1 2, Bo Wang 2, Cici Bai 1, Keyao Yang 1 2, Xu Ma 1 2, Liwei Zhang 1, Huan Sai 1, Yanbin Zhu 4 5, Xiuting Li 6 7
Background: The incidence and risk factors of secondary hip fractures is unknown. This study aims to evaluate the sex-specific incidence and risk factors of secondary hip fractures in elderly patients after hip fracture.
Methods: We did a systematic search of PubMed, Web of Science, Cochrane Library, Embase, MEDLINE, CBM, CNKI, VIP, and Wanfang Database from January 1, 2000 to August 1, 2025, for cohort studies that assessed incidence and risk factors among patients with secondary hip fracture. Eligible studies were appraised using the Newcastle-Ottawa Scale. The primary outcomes were incidence rates for secondary hip fracture, reported separately for man and woman. The secondary outcomes were risk factors for secondary hip fractures. Effect sizes included odds ratio (OR) with 95% confidence intervals (CI). Sensitivity analyses and subgroup analyses were performed to explore sources of heterogeneity. We used the population attributable fraction (PAF) and the grading of recommendations, assessment, development and evaluation (GRADE) to assess contribution and evidence quality.
Results: 19 eligible studies were included. The pooled incidence of secondary hip fractures among older adults was 10.63% (95% CI, 9.9%-11.4%), higher in females (14.94%; 95% CI, 0.123-0.178) than in males (9.89%; 95% CI, 0.083-0.116). Significant risk factors were reduced gluteus medius/minimus (G.Med/MinM) and gluteus maximus muscle density, reduced bone mineral density at hip, femoral neck, and intertrochanteric regions, osteoporosis, cognitive impairment, and calcium/vitamin D deficiency. Among these, G.Med/MinM density lower (moderate quality evidence, PAF, 6.54%, 95% CI 0.038-0.093), and calcium/vitamin D deficiency (moderate quality evidence, PAF,1.12%, 95% CI 0.007-0.016) were important factors.
Conclusion: Roughly one in ten older adults suffers a secondary hip fracture, with substantially higher rates in women. Muscle degeneration and inadequate calcium/vitamin D intake emerged as the most influential and potentially modifiable contributors. Targeted postoperative interventions addressing these factors may reduce recurrent fracture burden in aging populations.
Related in Vitamin D Life
Vitamin D and exercise after hip fracture surgery – far fewer deaths
1 in 3 died after hip fracture but only 1 in 14 if add Vitamin D and exercise – RCT April 2017
Same study as on this page- Resistance exercise combined with Vitamin D is great for seniors – meta-analysis July 2017
- Calcium and vitamin D supplements after hip fracture reduced death rate by 25% – Feb 2011
- 20 percent fewer male hip fractures if more Magnesium in the water – July 2013
Magnesium is needed to keep bone strength - Surgical outcomes are better for higher levels of Vitamin D – systematic review May 2015
Many surgery outcomes are better with higher levels of vitamin D - Overview Fractures and vitamin D
- 68+ pages with hip tracture in title as of Jan 2026
- See a hyperlinked list of all of them by clicking on hip-fracture at the bottom of this page
