Prostate Cancer Fought by Vitamin D in 4 ways
New insights into prostate cancer progression: A focus on vitamin D signaling
The Journal of Steroid Biochemistry and Molecular Biology Volume 261, July 2026, https://doi.org/10.1016/j.jsbmb.2026.107019
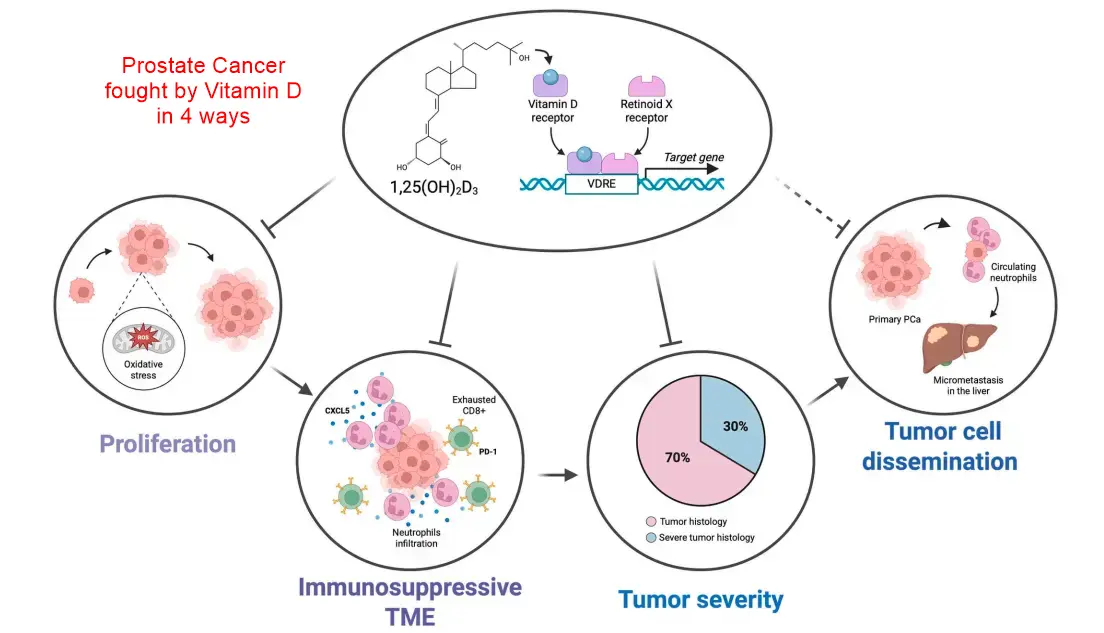
Prostate cancer (PCa) is one of the most frequent cancer in men of western society. Whereas the therapeutic options for localized PCa are efficient, those for advanced forms lead to resistance and are of a poor outcome. Thus, it is of utmost importance to understand the mechanisms underlying PCa progression to identify biomarkers predicting tumor evolution and novel therapeutic options. This review summarizes the current knowledge on PCa progression, treatments and preclinical approaches, with a specific emphasis on the role of vitamin D signaling.
6) Vitamin D and PCa treatment (clipped from PDF)
As PCa progression and aggressivity is associated with vitamin D deficiency, the relevance of treating patients with vitamin D arises. Long-term pharmacological vitamin D supplementation in patients suffering from PCa is limited, as doses required to reach anti-tumoral effects are often associated to hypercalcemia [108-110].
Therefore, pharmaceutical industries tend to develop vitamin D analogs with enhanced anti-tumoral effects and limited pro-calcemic potency. More than 4000 vitamin D analogs have already been synthetized and some exhibited promising anti-tumoral effects (e.g. Gemini-72 [Ill], Xe4MeCF3 [42] or inecalcitol [112,113]).
We recently explored in PTEN(i)pe-/- mice the effects of Gemini-72, a vitamin D analog with more potent activities than the natural ligand [77,111]. Besides the pro-apoptotic effect on senescent PECs, this analog impedes fibroblast activation, extracellular matrix remodeling and prostatic infiltration of immunosuppressive neutrophils through CXCL5 downregulation. Together with the results obtained in PTEN/VDR(i)pe-/- mice, vitamin D signaling appears as a negative regulator of CXCL5 expression. Single-cell RNA-sequencing also showed that a Gemini-72 treatment induces the loss of a subset of luminal-C2 cells, underlining its impact on tumor progression. However, remaining subsets of luminal-C2 cells exhibit higher pro-survival (PI3K/AKT/mTOR) and inflammatory pathways (NF-kB), explaining limitations of vitamin-based monotherapy in PCa [Ill].
An expanding body of evidence has highlighted the synergistic interactions between vitamin D and several antitumor agents, including taxane-based chemotherapy, thereby enhancing their anticancer activity [112-116]. The ASCENT clinical trial investigating high-dose calcitriol (DN-101) in association with docetaxel plus prednisone, has been terminated early due to a shorter survival in the treatment arm [117]. However, these results might be due to the use of a weekly docetaxel regimen, known to be inferior to the current standard every-three-weeks schedule, thereby confounding interpretation of the vitamin D effect. Another early phase clinical studies on PCa demonstrated that inecalcitol, a low-calcemic VDR agonist, can be safely combined with standard every-three-weeks docetaxel schedule and prednisone in mCRPC and is associated with encouraging PSA responses, supporting further evaluation of VDR-targeted therapies in this setting [112,113]. More recently, Len-Tayon and collaborators have shown that a vitamin D analog with a rigid side chain (Xe4MeCF3) used as a monotherapy had a limited effect on PCa treatment in chemoresistant IGR-Cap cells [42]. However, a Xe4MeCF3 and docetaxel co-treatment restores the che- mosensitivity. Subsequently, the promising synergic effect has been tested in vivo on CRPC PDX. In the same way as in vitro, the co-treatment limits cancer growth by targeting cancer progression pathways. These results position vitamin D co-treatment as a promising strategy to enhance the efficacy of advanced PCa standard of care therapies, effectively reducing cancer progression and overcoming untreatable multi-resistance.
Related in Vitamin D Life
- Overview Prostate Cancer and Vitamin D
- Prostate Cancer – Vitamin D – CYP27B1 – CYP24
- Low-risk prostate cancer treated by Vitamin D, Omega-3, etc.
- Prostate Cancers have 2.5 X more microplastics than non-tumor sections
- Prostate Cancer death 40 percent less likely if 40 ng level of vitamin D – Meta-analysis
- Prostate cancer reduced when 4000 IU vitamin D was added– Hollis RCT
Prostate Cancer Prevention
- Risk of Prostate Cancer 3X higher if very low Magnesium
- Prostate cancer risk reduced by Vitamin D (4000 IU daily)
- 2.5 X reduced risk of cancer in 70 year-olds by a small amount of Vitamin D, Omega-3 and exercise – RCT
- Prostate cancer risk cut in half by consuming Boron-rich food or water
- Men with High Omega-3 ratio 3 times less likely to have high grade prostate cancer
- The use of Vitamin D to prevent prostate cancer doubled in a decade
Prostate Cancer and poor genes (many cancers make the genes worse)
